December 1, 2014
What’s so good about the Nu-Schroth Scoliosis Method?
I recently took a call from a parent of an 11 year old diagnosed with scoliosis when she was 7 years old. During the past 4 years she has been under the care of an orthopedist who has dutifully monitored the child with x-rays during that time. At the last meeting the doctor recommended the child try some Schroth scoliosis exercises and recommended they find a local therapist trained in the 94 year old method. What changed? why did the Orthopedist suddenly recommend a nearly 100 year old method after 4 years of watchful waiting. This type of phone call has become quite common since the 2014 New York Times Article highlighting the Schroth scoliosis Method. The article is responsible for this resurgence in interest in non-surgical scoliosis treatment. In true American Fashion, we are not trying to extract out the “nutrient from the nutritious.” Let me explain, the Schroth method is an immersion technique and is provided in an in-patient setting. It includes up to 6 hours a day of therapy, massage, exercise and chiropractic. I spent two weeks at the clinic in 2008 and learned the method well. I knew when returning home I couldn’t offer an in-patient service and that I needed to modify the Schroth method to be suitable for U.S. consumption, and I didn’t want to water it down the way I knew would eventually happen. That’s when I came up with the “Nu-Schroth Method.”
The nu-schroth method uses the concepts I learned from the original Schroth method, but the concepts are applied with a 21st century take on rehabilitation. Lets face it, we’ve learned a tremendous amount since 1920, especially in the field or rehabilitation and the brain. The Nu-Schroth method uses contemporary rehabilitation methods like the Bosu ball, TRX training straps, HRV monitoring and vestibular rehabilitation. We teach the method in groups just the way Katarina Schroth did, and we modify activities of daily living the way Katarina Schroth did.
Here are 5 things that make the Nu-Schroth method the best even better than the Original Schroth Method for scoliosis;
1. The Nu-Schroth scoliosis method is taught so patients and families can do the exercises at home without needing to visit a therapists office daily. Exercises are broken down into Neurologic and Orthograde. Gait analysis is used as biofeedback to re-educate the gait of persons individually.
2. The Nu-Schroth scoliosis method uses Raster Stereography (a harmless imaging system) to monitor postural change, reducing the amount of harmful radiation exposure.
3. Nu-Schroth scoliosis method includes Chiropractic Neurology and manual therapy techniques which have been shown to improve the efficacy of exercises and postural restoration.
4. Nu-Schroth scoliosis method uses HRV monitoring to determine when patients should be resting, over training is a major cause of scoliosis progression
5. Nu-Schroth scoliosis method does their exercises to fatigue, then layers on complications to maximize results.
To learn more contact me directly at 1-800-281-5010 or visit scoliosissystems.com. 
November 9, 2014
What Makes Scoliosis get Worse?
Scoliosis is a genetic syndrome with a hallmark deformity of the spine, but it’s more than that. One way we identify genetic diseases is to study twin populations. Identical twins have the exact same genome, therefore genetic disease would be shared between the siblings, and that’s exactly what we see in scoliosis. However, these studies also show the severity of the disesse is variable, Twin studies have shown there is no question genetics play a role in developing the conditions, but differences in the direction and severity indicate there is more to it than just genetics. So what makes scoliosis get worse? Epigenetics, or factors beyond the genetics. Things like the environment and the health status of the individual. The environment can further be defined as the internal environment (metabolism) and the external environment (movement and posture). There is strong evidence that posture and movement are major factors influencing scoliosis progression. Newer science also supports hormonal, metabolic and neurological triggers involved in scoliosis progression. Our goal is to identify which trigger in which person may be a contributor to progression in that particular case. As you can imagine this is not easy to do, and requires a thorough history and exam in every case.
November 9, 2014
Should my child participate in Sports if they have scoliosis?
I recently interviewed a new patient and her family to find out her parents were encouraging her to join sports because she had recently been diagnosed with scoliosis. This is not uncommon in my practice, nor is the exact opposite, parents and doctors recommending no sports when curvatures become progressive. So which is it? Should children with scoliosis participate in sport or not? The first question that should come to mind is, what makes scoliosis curvatures progress? This is very important to understand; genetics cause the disease, and the environment is responsible for its progression. For our purposes, the “environment” is both internal (metabolism) and external (movement).
With that being said, here are few things to consider, firstly not all movement is created equal. If you think about “movement” as a large circle, then exercise is a smaller circle within that. Poor movement as well as poor postures have the potential to aggravate scoliosis, and to the contrary, movement can also be therapeutic, as is the case with good posture. Exercise is really no different, if the movements associated with the exercise are therapeutic or helpful then exercise is great, if the movements are imbalanced, limited,or unstable, then the exercise may aggravate the condition. We spend between 10 and 30 hours working on movement education with our patients. “Movement”includes exercising, as well as walking, running, stepping, sitting, standing, breathing, leaning, chewing, sitting, kneeling, lying etc.
Furthermore, exercise activates the sympathetic nervous system. Anytime you move, your sympathetic system has to dominate to bring blood to the muscles doing the work. When the sympathetics are dominating, the adrenal glands release cortisol, the heart rate becomes less variable, and digestion shuts down. Normally, the sympathetics are opposed by the parasympathic division of the autonomic nervous system, and the body returns to a state of resting and digesting. If a patient has a dominant sympathetic nervous system, it may be turned off after exercise, and lead to problems falling asleep at night (insomnia), they may be anxious, have tachycardia, have increased sweating, and decreased digestion to name a few. This is a major concern for scoliosis patients. Here’s why.
New research has identified a pathway responsible for asymmetrical bone growth related to increased sympathetic nervous system activity. Most of us are familiar with the sympathetic nervous system as the “fight or flight” division of the autonomic nervous system. Studies have shown scoliosis patients have a loss of brain influence over the sympathetics, allowing it to dominate even at rest. One way we can measure this is through the Heart Rate Variability.
Heart Rate Variability (HRV) is a measure of the balance of the sympathetic and parasympathetic influences over the heart. When the sympathetic system is dominating, the heart beat becomes less variable, meaning its rhythm becomes like clock work. This may sound good, but it’s actually not desirable because it makes the heart more susceptible to mis-beat. Studies show when athletes over train their HRV diminishes. Heart rate monitor technology allows us to easily measure the HRV allowing us to recommend rest days when exercise is leading to over training.
November 9, 2014
Hypothalamic Amenorrhea in Scoliosis
What is Hypothalamic Amenorrhea and how does it affect Scoliosis?
Studies confirm prolonged onset of the menstrual cycle is a risk factor for scoliosis progression. Termed Hypothalamic Amenorrhea, abnormal menses or lack menses can be caused by a lack of adequate body fat. This may be due to genetic predisposition, or due to either excessive exercise or low caloric intake. It’s important to understand why this happens. To put it simply, if the brain (hypothalamus) does not detect enough fat storage (Leptin signaling), it won’t waste energy on preparing the body for pregnancy. This can prolong the pubertal growth making these patients more susceptible to asymmetrical bone growth. Dietary and lifestyle changes should be considered in these cases. Supplementation that supports proper hormone function may reduce physiological dysfunctions associated with this condition.
September 8, 2014
Does my child have Neuro-skeletal Scoliosis?
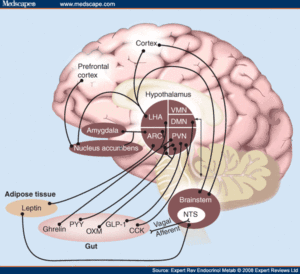
Neuro-skeletal scoliosis is a relatively new description which describes the pathophysiology of a particular type of progressive Scoliosis. (Neuro) meaning, under the influence of the nervous system, mainly the autonomic nerves which get their start in a part of the brain called the hypothalamus, and (Skeletal) pertaining to the growing bones, nerves and blood vessels all of which are involved in scoliosis.
The Hypothalamus is responsible for regulating our bodies homeostasis, which includes temperature regulation, feeding, satiety and hormonal balance. The Hypothalamus has direct links to the pituitary gland which is responsible for the onset or puberty and hormonal maturation. Nerve pathways from the hypothalamus follow along the sympathetic nerve chains to synapse on bone cells called Osteoclasts and Osteoblasts. Both of these cell types work to grow and remodel bone based on genetic coding, local sheer forces and neuropeptides directly from nerves.
Other Facts to Consider: Neuropeptides are tiny molecules produced and released by the nerve fibers as a consequence of local and global activation. Both Sensory nerves and motor nerve function influence bone symmetry and growth especially in adolescence. Global motor tone of the nervous system has influence over bone symmetry via the pontomedullary reticular formation (PMRF) pathways, which also influences vestibular function Heart rate and rhythm, sympathetic inhibition (sweating, pupillary dilation, and regional blood flow).
Why is it important to know if my child has Neuro-skeletal Scoliosis? When nerve function is disrupted, imbalanced or left uninhibited, or overactive, it results in asymmetry of bone growth and progressive scoliosis. Many of nerve imbalances can be improved, reduced or balanced by functional neurology approaches, physiotherapeutics and chiropractic methods.
How is Neuro-skeletal Scoliosis Diagnosed? A thorough clinical neurological exam may reveal neuro-skeletal motifs that can be treated clinically. Basic exams should include testing of: a. Reflexes b. Vibratory sense c. Ability to measure movement of the limbs d. Sensory appreciation of space, e. balance etc.
When Neuro-skeletal scoliosis is suspected, a more thorough exam should include:
1. Vestibular and oculomotor testing (VNG)
2. Somatosensory evoked potentials (SSEPs)
3. Brainstem Auditory Evoked Potentials (BAERs)
4. Functional assessment of the Pontomedullary Reticular Formation
5. Neurohormonal assessment (stress hormones, pituitary hormones, adrenal hormones, thyroid hormones (in adults)
6. EEG when cortical syndromes are suspected.
7. Chronic Upper Cervical Subluxation
What Treatments can be done if Neuro-skeletal Scoliosis is confirmed? Treatment objectives should be discussed with your clinician about your child’s specific condition. A multi-disciplinary approach may be necessary. In general, when patients have vestibular imbalances (studies show this is prevalent in 80% of Idiopathic cases), patient specific vestibular rehabilitation should be performed by a trained professional. That same patient may have neuro-hormonal issues, and may require care from an endocrine specialist. It is our opinion, a Functional Neurologist is the best managing clinician for these types of cases, however doctors of chiropractic and non-surgeon orthopedic specialists are often needed and therefore are also valuable in this regard.