July 7, 2017
Are Low Levels of Phosphorus Protective Against Scoliosis Progression?
Are Low Levels of Phosphorus Protective Against Scoliosis Progression?
Calcium and Phosphorus are at normal levels in Adolescent Idiopathic Scoliosis (AIS):
Calcium and Phosphorus are both important for normal bone mineralization, and can be mobilized to and from the blood stream and into the bone depending upon body homeostasis. Hormones (Parathyroid hormone and Estrogen) are mostly responsible for signaling when the minerals should be stored or released.
June 1, 2017
Scoliosis and Osteoporosis
Scoliosis and Osteoporosis
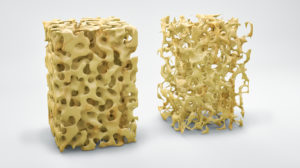
Did you know Osteoporosis is a risk factor for Scoliosis Progression? Typical Scoliosis braces hold the spine out of gravity and have a negative effect on bone density. Bone Density testing is a safe and reliable way to determine if bone density is a risk factor. In the event Osteoporosis, Osteopenia, or low bone density are confirmed, scoliosis bracing can exacerbate your condition. This is one reason scoliosis braces can be ineffective. It’s important to improve your bone density over time, and to use a brace designed to increase the effects of gravity.
May 25, 2017
Scoliosis, Osteoporosis and Vertigo in Clinical Practice
Scoliosis, Osteoporosis and Vertigo in Clinical Practice
Do you have one or more of the following; Scoliosis, Osteoporosis or Vertigo? Clinicians and Researchers have long reported that all three of these conditions can occur simultaneously. And now, new research may answer at least in part why patients with Scoliosis also have Osteoporosis and Vertigo.
May 16, 2017
Scoliosis Progression linked to Adolescent Version of Osteoporosis
Link Between Scoliosis Progression And Osteoporosis
It’s not surprising that osteoporosis has been found to be a risk factor for progression in adults with scoliosis, so it should also stand to reason that similar bone mineral deficiency can lead to scoliosis progression in adolescents.
Increased Risk Factor In Scoliosis Progression In Adolescents Linked To Similar Condition
The study entitled Osteopenia: A New Prognostic Factor of Curve Progression In Adolescent Idiopathic Scoliosis showed that adolescent girls with scoliosis were at greater risk for progression when they concurrently had osteopenia.

Osteopenia is the thinning of bone mass and is often considered the precursor to the more severe condition of osteoporosis that usually occurs later in life. Osteoporosis aka “Fragile Bone Disease” is characterized by a loss of bone mass caused by a deficiency in calcium, vitamin D, magnesium and other vitamins and minerals and is usually only thought to problem associated with menopause.
In this study researchers evaluated the bone mineral density (BMD) in the spine and hips of 324 adolescent girls with scoliosis. What they found was a correlation between a diminished BMD in girls with scoliosis to an increased likelihood of progression of their curvatures. The suggestion that diminished bone mineral density is a risk factor for progression of a scoliosis also does not come as a surprise.
What was surprising was the high percentage of adolescents with scoliosis that were also found to have osteopenia. Researchers estimated that as many 38% of young girls with scoliosis also have osteopenia, putting patients in this group at a significantly increased risk for curvature progression!

Table V. In this table researchers divided the girls into two groups based on the progression of their curves:
Group A. – Patients With Stable Curves
Group B. – Patients with Curve Progression
What they found was that over time the group that had progression of their curves also had a greater loss in bone density. Thus the evidence is clear that lower bone mineral density is a risk factor for progression.

Evaluation and Treatment Recommendations in Light of Study
As a result, doctors with Scoliosis Systems now recommend a Bone Density test (DEXA or DXA Scan) and a blood test for Vitamin D and Calcium Deficiencies to rule out this important risk factor for scoliosis progression in Adolescence. The results can be important in making dietary and supplement recommendations for those showing signs of osteopenia.
The authors also identified other risk factors for scoliosis progression which included a delayed onset of the menses. The research shows Ammenorhea and scoliosis progression are linked. The findings from both studies confirm hormones and bone health are directly related. Estrogen and Testosterone must be in balance for the menses to occur and continue regularly. Researchers routinely find testosterone to be in high concentrations in scoliosis adolescents, which leads to the interruption of the menses and the normal bone density.
Scoliosis tends to progress the greatest during the times of the increased metabolic activity such as the major growth spurt that occurs at the onset of puberty, also during pregnancy and menopause.
Weight bearing activity improves bone density, however this proves less effective in scoliosis patients. One reason this may be true is due to the asymmetrical loading to the bones in scoliosis curvatures.
Marc J. Lamantia DC
February 13, 2015
Neuro-Orthopedic Spinal Therapy; A novel approach to managing Scoliosis. PART 1
Have you wondered how conventional scoliosis methods came to be?
I often find myself pondering the origins of things, the origin of man, the origin of the universe, I’m especially perplexed by the origins of behavior. When we think about a conventional treatment in medicine, its nothing more than a behavior that is widely accepted and practiced and in not unchangeable.
So how did we get to the conventional behavior of managing scoliosis with surgery alone?
In 50 years we haven’t reliably sustained reduction in the amount of scoliosis surgeries, and continue to fuse the spines of young women with little concern about the longitudinal health of the individual. I work with many women with scoliosis, I always say my patients are usually either 13 year old girls or they’re 63 year old girls. Both have needs that are not being addressed by current conventional behaviors of their doctors.
Hormonal Effects of Scoliosis
I had a patient yesterday in Tampa, who will remain nameless, who has had an irregular menstrual cycle of the past year. She also of course has a scoliosis that is progressive. I asked the mom to please have some blood work done so we could potentially identify why her hormones were imbalanced. Scoliosis is related to hormones after all, it typically presents at puberty and tends to progress with increases in growth hormone exposure. The patient in being co-managed by an Orthopedist who would clearly prefer he were managing it alone, and a pediatrician. The Pediatrician said its “normal” to have an irregular menses the first year, and the Orthopedist says they’re in nothing that can be done other than surgery. These two recommendations are an example of how conventional methods may be potentially glossing over clinical findings that may now or later have a profound affect on the resulting deformity of the bone. Keep in mind, genetics have been shown to give us Scoliosis, but it the environmental stressors that lead to progression and worsening of the deformity.
Scoliosis Is A Multi-System Condition
Scoliosis is a unique condition that involves just about every system of the body including the skeletal system the muscle system, the nervous system, the hormonal system, the motor system, the oculomotor system, the gravi-ceptive (gravity sensing) systems, and the Sensory systems just to name a few. Its interesting to me that we have doctors for everyone of these systems, but when a patient has a curvature in their spine which we call “scoliosis”, our behavior is to revert back to a long ago decided method with origins long prior to our current knowledge of today.
The descriptions of Scoliosis date back to ancient times. Early Priest -Physicians thought it was an infestation by a demon leading to the hallmark curvature of the spine. Over time our understanding changed and so did our behavior. Undoubtedly the understanding changed long before the behavior did. This is of course how things evolve and we have to recognize where we are in any moment in time in contrast to a timeline that is much larger than our everyday thoughts admit to. Do you think we will be treating scoliosis the same way in 100 years from now? I hope not.
Over the past decade or so I have been immersed in clinical practice treating patients with scoliosis and hyperkyphosis. I happen to have hyperkyphosis myself and have a personal interest in what I do. I’m working on my posture right along side my patients, lucky them (tongue in cheek). I also fractured my spine when I was in my late twenties. My road to recovery was long and painful. I eventually, after about 5 years have found ways to move that don’t aggravate my pain and I continue to recreate with the best of them. Getting back to my point, over the past decade I’ve learned that the more you know, the less you know you know, and the more you want to know.
So my behavior has been changing over the past decade in regards to the conventions I choose to treat my patients, this is a direct consequence of changes in my understandings.
Neuro-Skeletal Impact on Scoliosis
For instance, the field of Neuro-skeletal Biology was first described in 2014. This branch of science investigates the relationship of the nervous system to the skeletal system. Now remember above I mentioned these two systems as being part of the many systems involved in the condition of scoliosis. This is all easily researched at pubmed.com, just put the keywords; neuro-skeletal biology. One study outlined the exact mechanism, to the best of their current knowledge and understanding of course, of how cells are activated to create the asymmetry associated with the spinal bones in scoliosis.
This is of course a new understanding and ultimately will change the behavior of those that are in the know. These studies identified divisions of the nervous system as being directly responsible for bony deformity in scoliosis. This changes everything, slowly. In our clinics we changed our behaviors immediately to include evaluation of the nervous system to identify if and when the nervous imbalance occurred.
Therapeutic Approaches To Diminish Neurological Imbalances Affecting Bone Growth
Our Conventions changed to include Heart Rate Variability monitoring and blood chemistry testing to name a few. We honed our focus in on methods designed to improve neuronal system balance and ultimately have developed a protocol that needs a name, and needs to be taught at the post graduate level to doctors with the necessary depth of knowledge in as many systems as they can, and then our Conventions will be one step closer to the reality.
I’ll be announcing a new seminar series in the coming months that will be for Doctors of Chiropractic exclusively. Our Neuro-orthopedic approach utilizes alternative methods to current conventional protocols. Your other physicians may or may not agree with our methods. Please invite to contact me directly, having your doctors start a conversation on your behalf can only benefit you.
For those of you practitioners interested in learning about our future scoliosis treatments Click on This Link to learn more.