April 4, 2014
Scoliosis Affects the Entire Body
Scoliosis Affects are on the Entire Body
Scoliosis is generally viewed as a lateral curvature of the spine with an axial twist that causes a distortion of the ribs. Current research shows that idiopathic scoliosis is a multifaceted disease that compromises five of the body’s systems: digestive, hormonal, muscular, osseous (bones), and neurologic.
Scoliosis affects the entire skeletal system including the spine, ribs, and pelvis. It impacts upon the brain and central nervous system and affects the body’s hormonal and digestive systems. It can deplete the body’s nutritional resources and damage its major organs including the heart and lungs.
Some factors that can cause scoliosis include: cerebral palsy, birth defects, muscular dystrophy and Marfan syndrome. However, 80% of scoliosis is idiopathic (unknown in origin).
According to the International Scoliosis Society, one in nine females and a smaller percentage of males have some sign of scoliosis. Approximately 4% of the general population is affected. While the average patient is between 10-15 years of age, many adults suffer from this disease as well.
Conditions arising as a result of scoliosis include rib deformity, shortness of breath, digestive problems, chronic fatigue, acute or dull back pain, leg, hip, and knee pain, acute headaches, mood swings, and menstrual disturbances.
Scoliosis is a progressive condition that can continue to progress even after skeletal maturity. Millions of scoliosis sufferers are routinely misinformed about the accelerating nature of their spinal curvature progression.
April 4, 2014
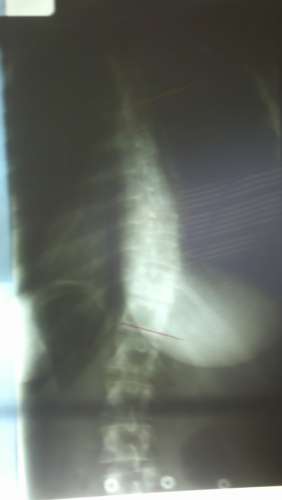
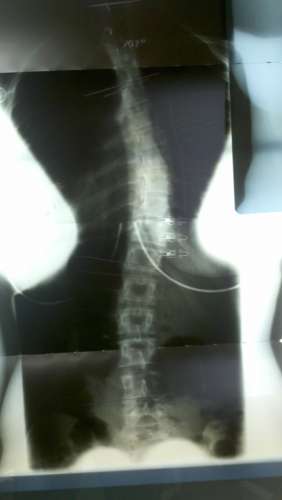
Scoliosis Systems Patient Avoids Surgery
 |
 |
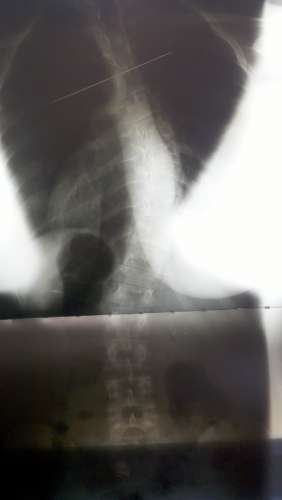 |
| 36° Initial | 2 in brace 30° | 34° 2 + yrs out of brace |
February 28, 2014
SpineCor treatment for Juvenile Idiopathic Scoliosis
Juvenile idiopathic scoliosis usually presents itself between the ages of 4-11 years. When scoliosis presents itelf early in life the curvatures are often small when diagnosed and often are not referred for good non-surgical intervention. The tendency is for everyone including the Orthopedic or Pediatric doctor to recommend observation until the curvature worsens. In my opinion this is a collossal mistake and often results in untreated scoliosis curvature progression. Those that are diagnosed at five years or younger have a high chance of progression to a large curve, with additional pulmonary and cardiac complications possible. Evidence suggest early intervention can reduce the effects of scoliosis, and may be capable of silencing the gene expression responsible for progression.
Evaluating for all epigenetic envirnomental triggers can difficult, however we think evaluating for the top 4 makes good sense, 1, neurologic imbalance (vestibular, autonomic, cortical), 2, Metabolic/dietary 3. Hormonal, 4. Orthograde (movement and postural imbalances).
Treatment options should be discussed with the family and a long term plan should be crafted. This age group responds well and quickly to good non-surgical scoliosis management. Each catagory should be considered and weighted for importance by your clinician.
Bracing is also an important treatment in this patient population. The only problem is this group can need treatment for a decade. Rigid bracing is not practical and may be detrimental to the the health of the patient in other ways. In 2002 I discoved a Canadian doctor using a flexible dynamic brace which solved many of the problems we see with rigid braces. To learn more about flexible bracing click on the link below.
February 28, 2014
New Study Suggests Lowering Threshold for Scoliosis Treatment to 20 degrees
OBJECT
The identification of Chiari malformations Type I (CM-Is) has increased in recent years, commonly during MR imaging for evaluation of a possible cause of scoliosis. The treatment of this abnormality remains controversial, and the expected success of treatment is unclear. The goal of the present study is to evaluate the effects of a craniotomy for CM-I decompression on scoliosis in children and adolescents.
METHODS
The authors conducted a 10-year retrospective review of pediatric patients who were found to have a CM-I during evaluation for scoliosis. Seventy-nine patients were identified, ranging in age from 6 months to 18 years (median 12 years). There were 42 girls (54%) and 37 boys (46%). All were noted on MR imaging to have hydrosyringomyelia of the spinal cord. Forty-nine patients had curvatures less than 20° prior to treatment. The other 30 patients had curves ranging from 25° to 80° and underwent orthopedic follow-up and treatment. None of these patients were referred for specific neurological complaints, but 12 (16%) had neurological signs on physical examination. All were treated with a craniocervical decompression in a standard fashion. Follow-up ranged from 6 to 93 months with a median of 35 months. Magnetic resonance images obtained at 6 months postoperatively and serial standing anteroposterior spine radiographs were used to evaluate outcomes.
RESULTS
On the MR images obtained 6 months postoperatively, 70 patients (89%) had a significant reduction in the syrinx with an associated ascent of the cerebellar tonsils. Persistent large syringes were treated with reoperation in 6 patients, and shunts were inserted for hydrocephalus in 2 patients. None of the 49 patients with curves less than 20° had progression of their curvature postoperatively. Of the 30 patients with curves greater than 25°, 9 had no change in the scoliosis or had a reduction in curve magnitude after Chiari decompression. This group required no further therapy and was effectively treated by Chiari decompression alone. Twenty-one patients required further scoliosis treatment after Chiari decompression; 12 required orthotic treatment, 11 received spinal instrumentation and fusion surgery, and 2 received orthoses followed by fusion and instrumentation. The severity of the curvature beyond 20° did not predict the need for spinal surgery.
CONCLUSIONS
This large series reports on the efficacy of treatment for scoliosis associated with a CM-I and syrinx in children. A CM-I decompression alone was adequate treatment for mild scoliosis of less than 20°. Patients with scoliosis greater than 20° required bracing and/or spinal fusion surgery 70% of the time in addition to the CM-I decompression.
February 9, 2014
Scoliosis Treatment Success
Presentation: A 62 year old female presented herself without referral for the examination. Her medical history included multiple recent falls, adult progressive scoliosis and a possible diagnosis of Multiple Sclerosis from her medical neurologist.
Observations posture reveal chronic towing of the spine to the right, shuffling gate with wide stance and the need to constantly hold on for stability.
Exams: a comprehensive neurological exam was performed including a sensory motor exam, a cerebellar and brainstem cranial nerve exam with appropriate testing of vestibular and oculomotor function. Clinical findings were nomometric in regards the motor examination. Ranges of motion were restricted in an age appropriate manor and sensory exam was further unremarkable. Vidoe Electronystagmography allowed for the evaluation of the vestiublar Cranial nerve portion, and as well as oculomotor testing. Upon vision denial testing in the upright seated posiition the patient presented with a non fatiguing right beating nystagmus with not tornsional or vertical component. The nystagmus was not visible without vison denial goggles. Oculomotor testing revealed findings of an adduction lag in the left eye during optokinetic stimulus. Xrays of the spine revealed an atypical towering scoliosis with severe lumbar disc degeneration and hyperostosis of the weight bearing joints.
Chiropractic evaluation included stereo views of the full spine posture and radiological views of along the X,Z, and the Yz axes and were reviewed in clincial context to recent MRIs provided by the patient. An occipito-atlanto-axial misalignment was measured. Reflexive retraction of the lower limb in non weight bearing supine posture was observed, and nerve root swelling with associated allodynia was localized by palpation at the c1 nerve root region. furhtermore, nucheal rigidity on the ipsilateral posterior neck musculature ws observed.
Differential Diagnosis: Cerviical Subluxation complex, Adult progressive scoliosis and associated osteoarthritis, left unilateral vestibulopathy, demeyelenating of the medial longitudinal fasicular tract from the right adbucens nucleus to the left oculomotor nucleus. CSF flow disruption.
Plan: Follow up clincial testing is necessary. Xrays, caloric testing as well as repeat oculomotor testing is necessary to reproduce earlier findings. Chiropractic intervetion can begin immediately to reduce upper cervical spine dysfunction and C1 nerve root irritation. The patient is recommended to wear a spinal orthosis designed to improve dynamic control of the trunk and spine. Conservative treatment for vestibular and oculomotor findings.